There is little research conducted on sacral agenesis, and when it is conducted, it is sometimes unfortunately influenced by researcher bias or assumption due to the fact that they may have little contact with this community of individuals. When the medical profession relies upon a study or two to make decisions with regard to treatment, the results can impact the population of those with sacral agenesis in a negative way.
An example is a 2014 study in the Pan African Medical Journal here This article is accessible globally because it is included in the National Institutes of Health public database. It discusses a decision about disarticulation at the knee for a child with sacral agenesis and characteristic webbing and fused, bent knees. As one of the only current studies to address this surgery, the article states that a determination was made not to provide disarticulation surgery because
- there was no possibility of ambulation.
- the bent knees provided sitting stability and therefore should not be removed.
In both cases, these statements are incorrect assumptions. Another rationale that has been reported for not doing this surgery is that the main artery of the leg takes the shortest course through webbing behind the knee so disarticulation would compromise blood supply. Again, those with SA/CRS have experienced successful surgeries despite the pathway of the main artery.
The decision to disarticulate webbed, fused, bent legs is an individual decision, but it does offer many benefits. For a list of considerations, see this chart. Those who have had this surgery report improved mobility, ease of seating, improved wheelchair fitting, reduced issues of blood clots in lower legs, and increased ease of self care and independence overall. In not a single case is there any report of reduced sitting stability. In fact, the disarticulation allows the legs to be brought to a forward position, adding stability to wheelchair seating that was previously precarious due to the wide seat necessary to accommodate the width of the knees. The narrow wheelchair seating afforded by at-knee disarticulation additionally reduces the shoulder strain of pushing a wide chair where the wheels are not in-line with the shoulders. In regards to concerns over blood supply, the disarticulation surgery is accomplished without compromise or cutting of the artery. It is maintained in the skin flap for closure of the end of the knee.
Some individuals with straight, fused legs also seek disarticulation at the knee for the same reasons. The seating accommodation of knees that won’t bend is often problematic and worsens over time as legs grow longer. Two approaches, either stopping growth of the legs before the length becomes problematic or disarticulation at the knee are viable options for improved mobility. For more information, see “Orthopedics” on this site. here
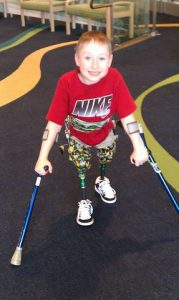
It is often not anticipated that these surgeries will allow for ambulation, but in many cases with the use of prosthetics the children who did not walk previously do walk after disarticulation surgery. They may not be life long walkers, but they often walk for a number of years and gain the advantage of being able to determine the most efficient mobility option for their daily lives.
While the choice for disarticulation is a personal one, it should be made based on accurate information. Unfortunately the study above makes an assumption that was not validated by research with individuals who have had the surgery.
